St. Luke's Health joins CommonSpirit.org soon! Enjoy a seamless, patient-centered digital experience. Learn more
Neck or lower back pain can be frustrating, especially when you don’t know the cause. Did you pull a muscle when you twisted the wrong way last week, or did you sleep in a weird position? If the pain radiates throughout other parts of your body, it might be due to a herniated disc.
Vertebrae are small, interconnected bones that house the spinal cord. Discs sit between each vertebra to help cushion and support them. Discs have two main components: a nucleus in the center and a tough outer shell. They keep your vertebrae from compressing nerves in the spinal cord when you move. As you age, the protective layer can wear down, and the nucleus can bulge out and compress spinal nerves. Most disc herniations occur in the lumbar spine (the lower back), but they can also occur in the cervical spine (the neck).
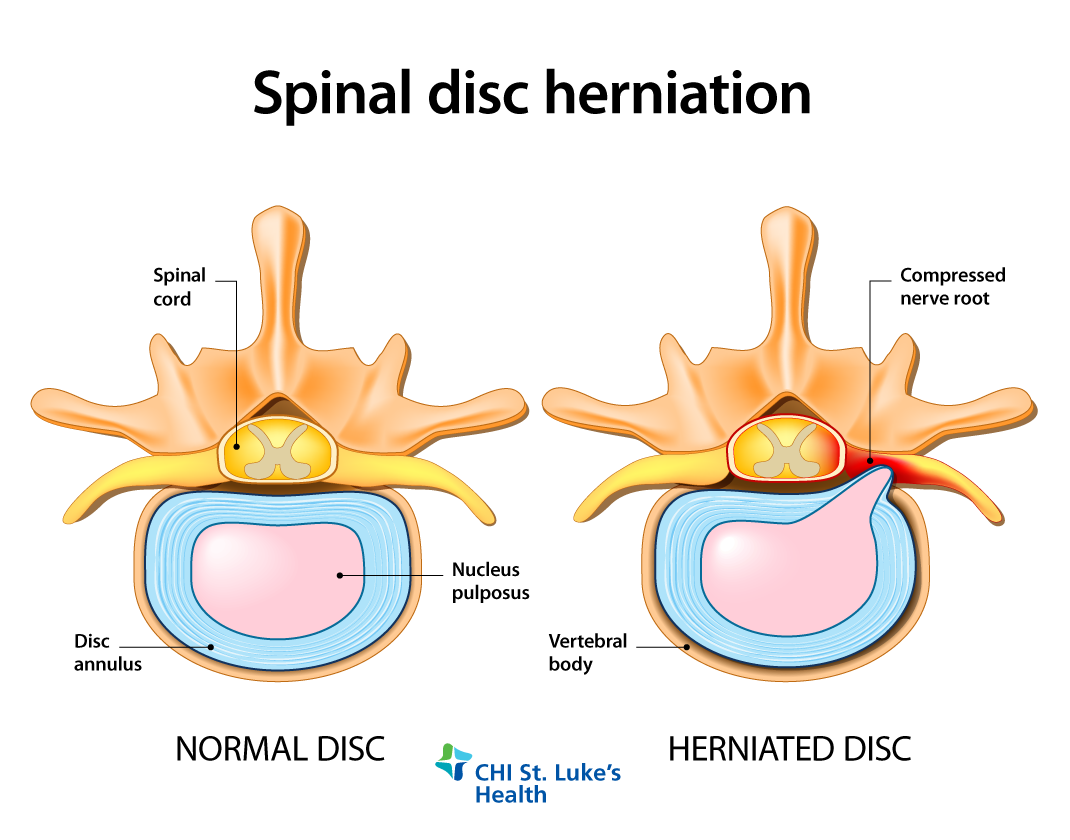
The symptoms of a herniation can vary widely depending on the location of the disc and the degree of displacement. If it occurs in the neck area, you might experience pain, numbness, burning, tingling, or weakness in your arms and shoulders, while a slipped disc in the lower back might produce the same kind of symptoms in the legs. If the disc isn’t pressing on any nerves, you might have mild back pain or even no pain at all.
After diagnosis, your doctor will likely recommend treatments such as anti-inflammatory medication, muscle relaxants, pain relievers, and physical therapy. They will also suggest avoiding any movements or activities that put a strain on your body for a few weeks. If these treatments don’t alleviate your pain after an extended period, they might suggest an epidural steroid injection or surgery.
You might be a candidate for surgery if you’re relatively healthy and:
If chronic pain is affecting your life, schedule an appointment with a Baylor St. Luke’s Medical Group orthopedic physician. From diagnosis through recovery, our team has your back.
Sources:
AANS | Herniated Disc
AANS | Anatomy of the Spine and Peripheral Nervous System
Looking for a doctor? Perform a quick search by name or browse by specialty.