St. Luke's Health joins CommonSpirit.org soon! Enjoy a seamless, patient-centered digital experience. Learn more

There is a glimmer of hope as experts look toward the future and the end of the COVID-19 pandemic. A vaccine is in the works, new treatment options are in clinical trial, and we’re learning more about the virus every day. So let’s take a look at the possible scenarios of how the pandemic may unfold over the next couple of years.
Using data from past flu pandemics and studying the behavior of this and similar viruses, researchers at the Center for Infectious Disease Research and Policy at the University of Minnesota mapped out three possible journeys for this pandemic.
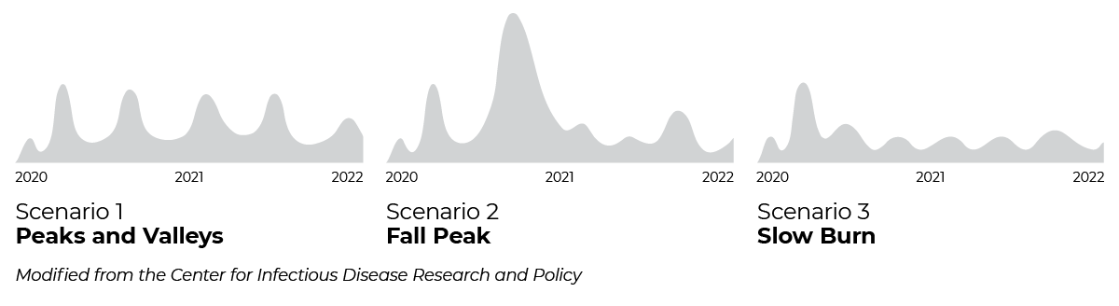
The first scenario involves a series of consistent peaks and valleys. The second predicts a seasonal peak of cases, similar to what occurred about a century ago with the Spanish flu. The third depicts a sharp peak of cases early on with a series of smaller ups and downs as cases decline.
Keep in mind: There is no one-size-fits-all projection that we can apply across every state in America. We also have to consider the different features and climates of each area, as well as the protocol that’s in place to slow the spread.
So let’s dive deeper into what would happen if certain controls were in place.
The Center for Communicable Disease Dynamics at the Harvard T.H. Chan School of Public Health mapped out how certain factors may affect the spread of COVID-19.
Every county has implemented various measures to flatten the curve, the purpose of which is to avoid overwhelming hospitals. These initiatives include social distancing, establishing stay-at-home orders, wearing masks, contact tracing, etc.
Once cases begin to decline over a period of time, leaders can loosen restrictions until cases begin to rise toward a threshold dependent upon hospital capacity. With social distancing interventions, it would look a little something like this:
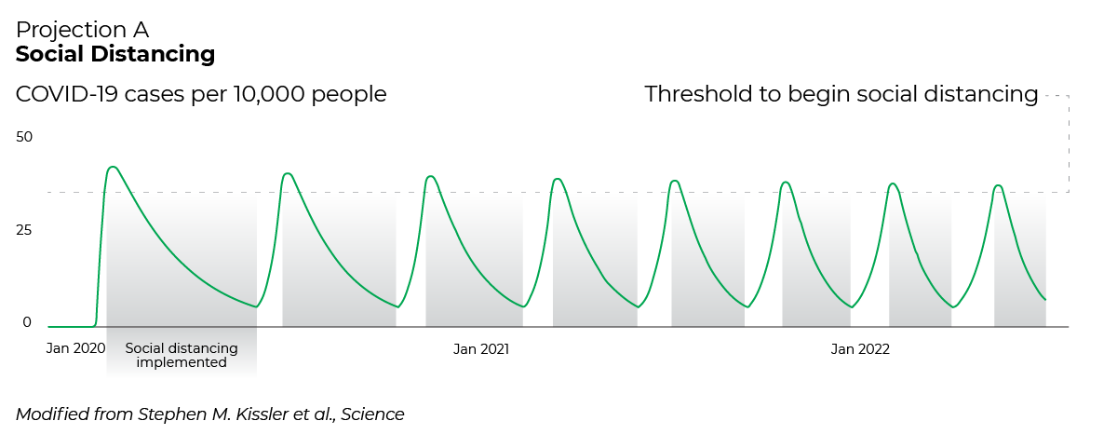
The green bars represent when social distancing guidelines are in place. As the number of cases fluctuates, these guidelines are implemented and removed with the ebb and flow.
But what if the changing seasons have an effect on COVID-19, demonstrated in Scenario 2 above? We might witness a minimal decline in spread during warmer months and an increase during colder months, slightly changing the trajectory to something like this:
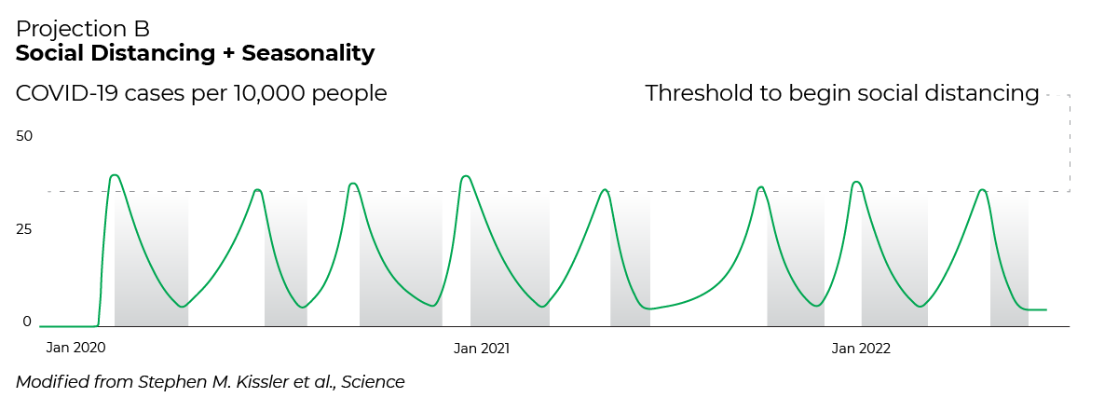
What if a community were able to double the critical-care capacity of local hospitals with additional resources? Leaders could lift restrictions for longer periods of time, leading to more pronounced ups and downs:
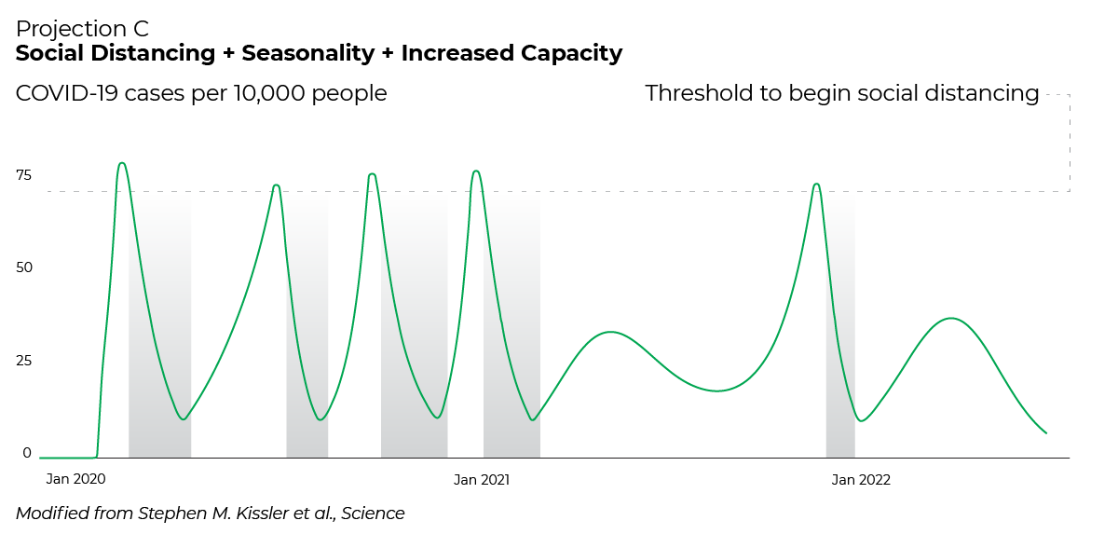
But wait! There’s another factor to consider.
Studies suggest that when someone overcomes COVID-19, they develop a level of immunity to the virus. This means it’s unlikely for people who have had the virus to contract it again. As the local population gradually develops herd immunity, we can better contain the spread of the virus throughout the community. Safely building herd immunity without a vaccine requires a controlled increase in social interaction.
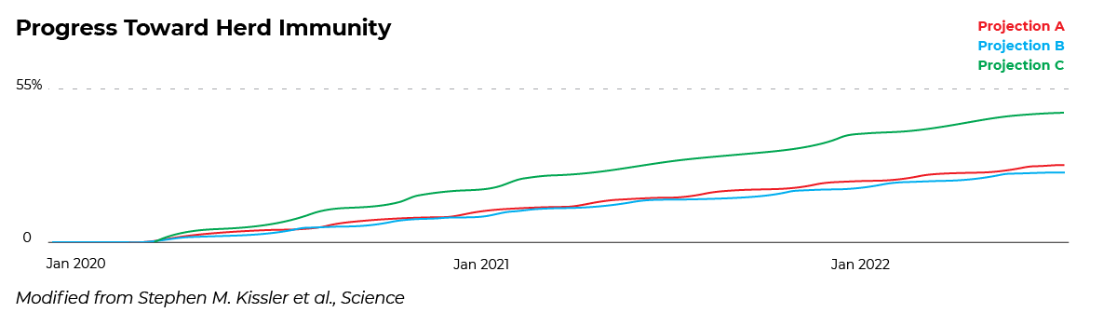
In these particular models, the herd immunity threshold is 55% of the population. In other words, 55% of the community would need to develop immunity in order for the virus to stop spreading without other controls, like social distancing, in place.
Here’s what herd immunity may look like for each of the above projections.
No matter how the pandemic unfolds, St. Luke’s Health is here to provide the care you need. Having established the highest safety protocols, our clinics and hospitals are open for in-person appointments so you can keep your health on track. For minor injury and illness, you can schedule a virtual visit with a Baylor St. Luke’s Medical Group physician.
Sources:
AAAS | Projecting the transmission dynamics of SARS-CoV-2 through the postpandemic period
New York Times | This Is the Future of the Pandemic
Looking for a doctor? Perform a quick search by name or browse by specialty.